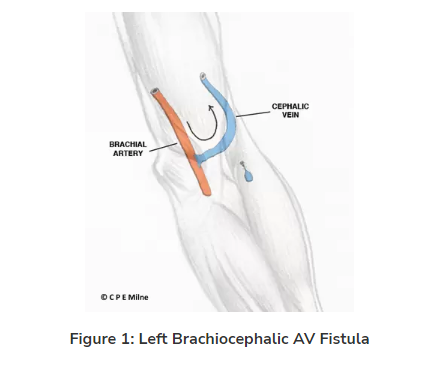
Preparing for the Procedure:
Prior to AV fistula formation, a duplex ultrasound of the arm veins is done to look for veins of suitable size to use. The arteries are also assessed to ensure that they are of adequate size, free from disease, and will provide adequate 'inflow' to the fistula once formed. A baseline set of blood tests will also be done.
Unless otherwise specified, all regular medications are continued prior to the procedure. Mr Milne will give you specific instructions regarding anti-platelet medications (e.g. aspirin, clopidogrel), anti-coagulant medications (e.g. warfarin, Eliquis), and any medications taken for diabetes.
Bring a small suitcase with you to the hospital in preparation for an overnight stay.
Description of the Procedure:
The procedure is usually performed under general anaesthetic. In high-risk patients, it can be done under local anaesthetic +/- sedation. A small incision is made in the arm, at the level at which the vein is to be joined to the artery. In most cases, the incision is just above the wrist or in the elbow crease. In the case of a transposition brachiobasilic AV fistula (~5% of cases), the incision is longer, and extended along the length of the basilic vein (on the inside of the arm above the elbow).
The vein and artery are carefully dissected. Clamps are applied to the artery to allow a small section to be opened. The mobilised vein is then sewn on to the artery forming a join (anastomosis). The vessels are flushed to remove debris. The clamps are then released, restoring blood flow to the artery and commencing flow through the fistula and in to the superficial vein. The anastomosis is checked for haemostasis.
The incision is closed with layered sutures, and the skin is closed with a dissolvable stitch underneath the skin. Occasionally, a small drain is left in the wound, and this is usually removed the next morning.
Following the Procedure:
You will be transferred to the vascular ward for monitoring after the procedure.
You may eat and drink after 2 hours.
On the first day after the procedure, it is usual to have some mild discomfort and bruising at the site of the operation. This usually settles within a few days.
Most patients are discharged home on the morning following the procedure. In the less common case of a brachiobasilic AV fistula formation, an additional night is usually required to monitor the wound.
You will be scheduled for a review appointment with Mr Milne 4 - 6 weeks after the procedure. At this stage, for a standard AV fistula which has been made with an artery and vein of good calibre, it is usually ready to access for dialysis. A duplex ultrasound is performed at the same visit to check the size of the vein and the flow through the fistula.
Travel:
It is generally advised to wait at least 1 to 2 weeks before driving a motor-vehicle. Use of the steering wheel should be unrestricted when driving.
You may fly interstate after 1 week, and may fly internationally after 4 weeks. If flying, it is important to stay hydrated and walk around the cabin regularly.
Possible Issues Following the Procedure:
- Bleeding:
- Occassionally, a collection of blood (haematoma) forms at the site of the operation. This is usually self-limiting, and is gradually absorbed by the body over several weeks.
- Rarely, a trip to theatre is required to evacuate a larger haematoma.
- Any external bleeding or large focal swelling of the wound should be reported to Mr Milne immediately.
- Infection:
- The risk of an infection involving the operative site is <5%. This type of infection usually resolves with a course of oral antibiotics.
- Thrombosis (clotting off) of the fistula:
- In the first 30 days, if the artery and vein are of good calibre, this is a rare event (~1%) .
- The risk of thrombosis is increased if the artery &/or vein are suboptimal (i.e. small or diseased).
- Failure to mature:
If the artery and vein are of good calibre, the fistula will mature to be ready for dialysis in >95% of cases.
The risk of encountering issues with maturation is increased if the artery or vein are suboptimal (i.e. small or diseased). There are most often treatment options to assist the maturation process.
- Re-intervention:
- In the long-term (months to years), narrowings may develop in the fistula which restrict the flow of blood. If the flow reduces to a critical level, the fistula can thrombose.
- There is almost always adequate warning to treat these narrowings before they cause the fistula to block, as they will impact on the efficiency of dialysis. If there is trouble with dialysis, it is important to contact Mr Milne urgently.
- Most often, narrowings can be treated with minimally invasive angioplasty (ballooning) of the fistula. Occassionally, an opensurgery revision of the fistula is required, which most often involves using a piece of vein to 'patch out' or replace a narrowed segment of the fistula.